AMY WEEDEN
You may have noticed the terms “urothelial cell” or “urothelium” being used in urinalysis, cytology, or histology reports over the last several years. There has been a shift in human medicine and, later, in veterinary medicine from the use of transitional epithelium to urothelium to describe the specialized stretchy epithelial tissue that lines the renal pelvis, ureters, bladder, and proximal and mid-urethra.
I’m not certain what prompted the alternate nomenclature, and there does seem to be some debate about which name is preferable. Urothelial is more descriptive of location, but this could be confusing, as urothelium is not present throughout the entire urinary tract (e.g. the renal tubules are composed of cuboidal to columnar epithelium, and the distal urethral lining is composed of squamous epithelium).
Transitional epithelium is specific to the structure and function of the epithelium and is descriptive, as this epithelium can have quite a variable appearance in health (i.e. transitional). However, there is some debate among pathologists about the structure of this epithelium, which is beyond the scope of this newsletter. Another pro in the “transitional epithelium” column is that this term has been in common use for many decades, and it is probably the term most veterinarians use.
Which term is superior may be up for debate, but you can expect that “urothelium” will become even more prevalent in the literature and in your reports (unless we decide later that we need a new term for it!).
Regardless of what you decide to call the epithelium, carcinomas arising from the transitional epithelium or urothelium can be challenging to diagnose by non- or minimally invasively means in some cases. Confounding secondary inflammation, lack of sufficient criteria of malignancy, and cellular degradation in urine sediment or traumatic catheterisation samples are all possible barriers to a confident cytologic diagnosis.
The case that follows is an excellent example of a diagnostic transitional cell/urothelial cell carcinoma (TCC / UCC) cytology with a somewhat unusual presentation on physical exam.
Clinical history:
An adult female large breed dog presented for bleeding from the vulva, and nodular lesions were identified on vaginal exam and swabbed for cytology.
Cytology findings:
Images from the excellent, highly cellular sample are shown. Cohesive clusters of highly atypical epithelium were identified. The features of the epithelium were not particularly distinctive with the exception of rare large magenta cytoplasmic vacuoles, also known as Melamed-Wolinska bodies. While eosinophilic inclusions can be found in the cytoplasm of other types of neoplastic epithelial cells, the appearance of this particular vacuole can aid in confirmation of urothelial cell origin in some cases. Based on this feature and the degree of atypia in the epithelium, urothelial carcinoma was the presumptive diagnosis.
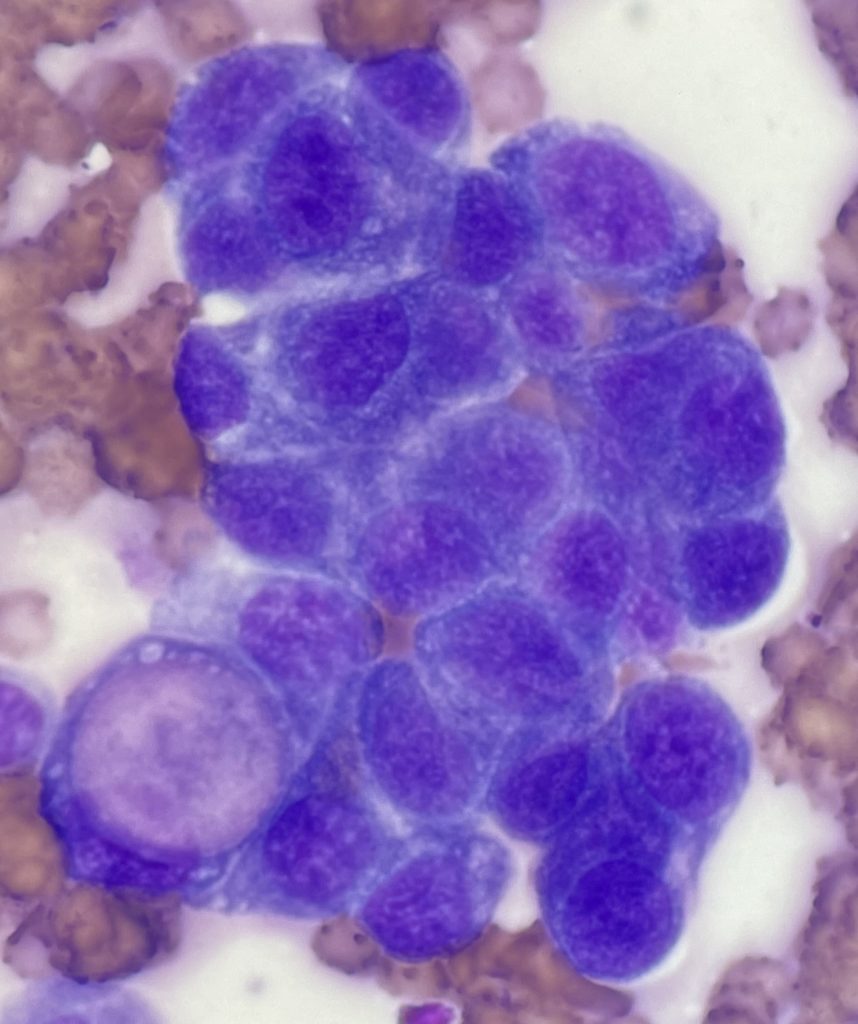
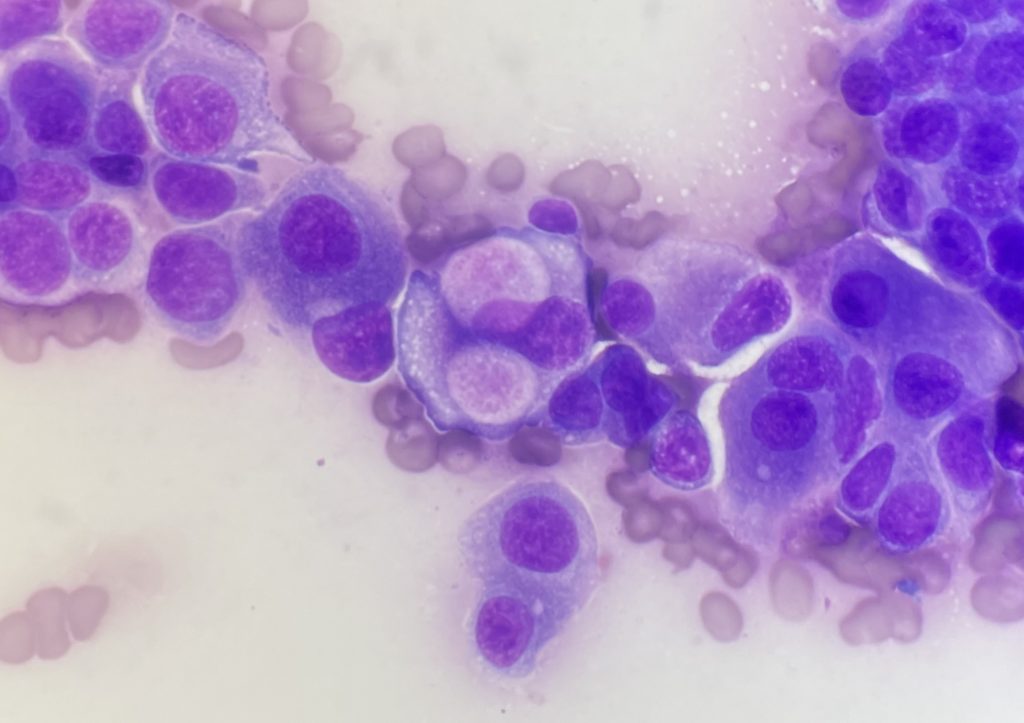
Further investigation revealed a urethral mass, and TCC/UCC was confirmed with histology. The nodular vaginal lesions were determined to be metastases.
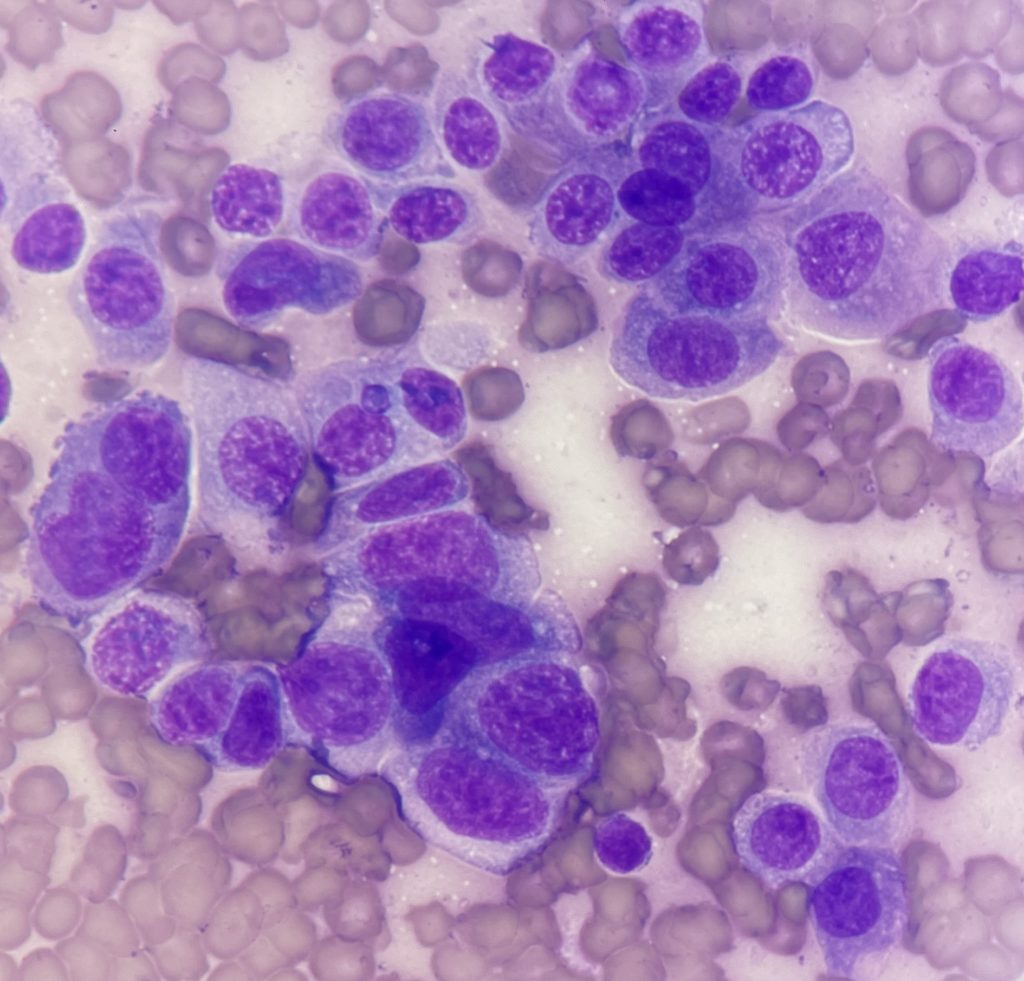
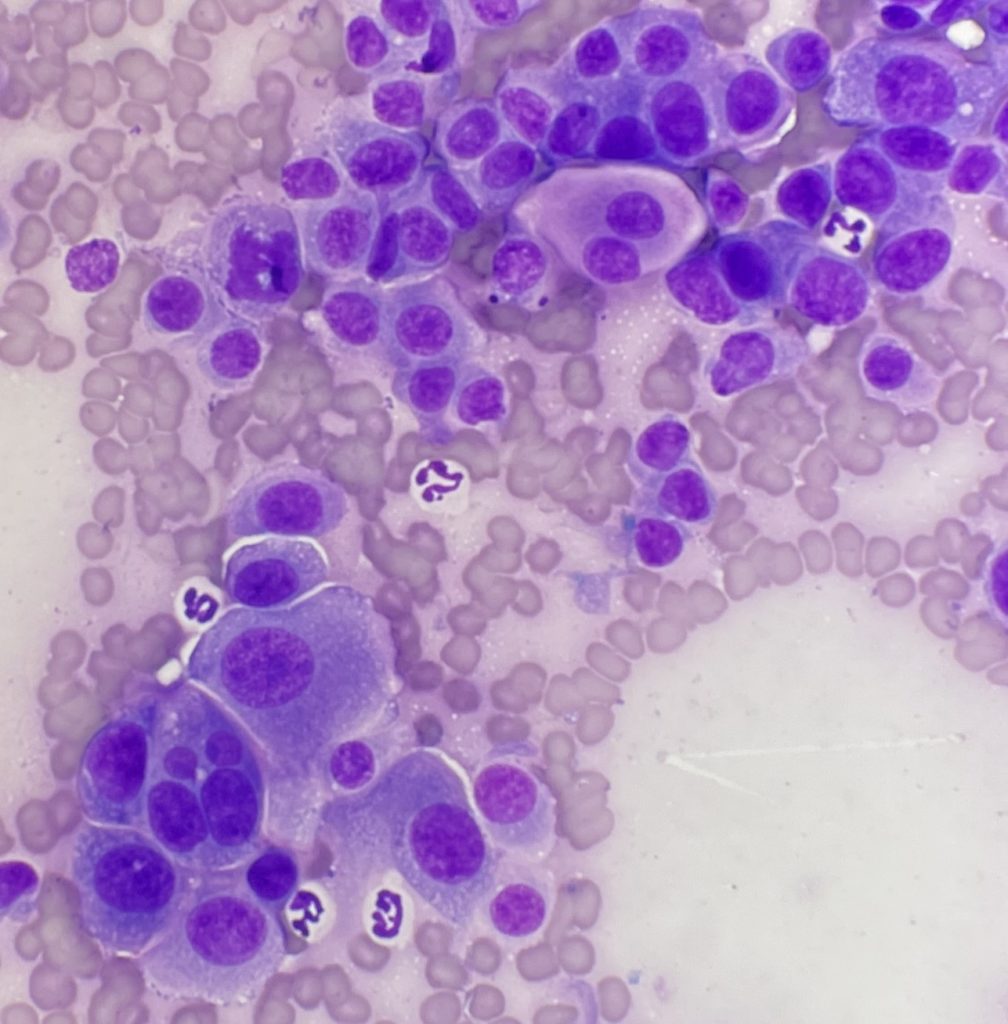
These images contain cells with frequent criteria of malignancy. How many can you identify? (Note that there is some variation in the literature regarding what constitutes criteria of malignancy.)
Discussion:
Atypical features in the urothelial carcinoma cytology:
> Marked variation in nuclear sized (anisokaryosis)
> Coarse or open chromatin pattern
> Variable nuclear to cytoplasmic ratio
> Bi- or multi-nucleation (a large cell near the bottom left of Figure. 4 contains four nuclei)
> Nuclear moulding / crowding
> Multiple nucleoli (may be difficult to see in small images)
> Only one mitotic figure is shown in these images (Figure. 4). Mitotic figures alone don’t necessarily indicate malignancy, but increased numbers or morphologically abnormal mitotic figures are suggestive.
Thank you to Nicola Dunlop at Helensburgh Veterinary Clinic for the interesting submission and excellent cytology smears.